How much does glucose tolerance – or intolerance – matter to a physique athlete? With all the talk in T-mag and the T-mag forum, it's high time we covered some basics.
Many of us realize that obesity is related to poor carbohydrate handling in Type II diabetics but how about the rest of us? Why is insulin a "Jekyll and Hyde" hormone that can be friend and foe? Why does John Berardi panic over caffeine's effects on glucose tolerance? (That's partly tongue-in-cheek, John!) Why do I keep harping on the importance of nutrient timing/ temporal nutrition? How can we manage insulin to our aesthetic and healthful advantage? Why do I keep asking so many questions?
There are still so many questions surrounding glucose tolerance for bodybuilders that the whole issue can become, well, intolerable!
Let's answer at least a few of these difficult questions. And hey, let's do it with a few anecdotes so you don't all fall asleep!
First, many readers know that insulin is our most anabolic hormone. But how anabolic is it? Well, once upon a time, prior to a protein supplementation/ bodybuilding study, a pretty small and fatigued looking research subject showed up to volunteer. He stated that he "used to be big" and that he was a Type I diabetic (no endogenous insulin production) and hadn't bothered to take his insulin much lately. He then explained that he had reportedly lost over 30 pounds in the prior 2-3 months. Dude. Do you enjoy having Mrs. Butterworth's syrup for blood? How about that nice blurred vision, constant peeing, thirst, hunger, and all the other dangerous risks of diabetes?!
Needless to say he was forwarded to healthcare authorities and was unable to participate in our protein research. No amount of supplementation was going to help this guy. But you can see the power of insulin. Take it away and boom! You're small.
Conversely, many of you are also aware of the fat-building power of insulin. You probably also know about the rising state of diabetes and Syndrome X in the U.S. In Temporal Nutrition, I mentioned that I've been putting in a lot of time at a local medical center that's had amazing results using Metformin with over-fat, hyperinsulinemic (insulin-resistant) patients.
Although they have near-normal blood glucose concentrations, they exhibit absolutely nutty insulin levels to keep their blood sugar in check. This kind of insulin resistance, once thought of as an adult issue like Type II diabetes, is happening frequently now with kids too (as is Type II diabetes in general nowadays).
The nutritional state of western society is going to hell in a sugary hand basket. By correcting the metabolic situation with drugs, however, these patients actually lose 1-2 pounds, presumably of fat, per week with few other lifestyle changes. Wow!
Looking closer at the mechanisms behind such power, we see that adipocytes (fat cells) possess an ability to respond to insulin with a massive 30-fold rise in glucose uptake (and subsequent lipogenesis) while myocytes (muscle cells) respond with just a 3.2-fold increase.(2) Hence, spiking your insulin levels repeatedly with refined carbohydrate or carb-plus-fat meals (e.g. kids' cereals, donuts, pancakes, white bread with butter, pasta with margarine and cheese, etc. etc...) builds (or preserves) more fat than it does muscle.
 |
| Figure 1. Proposed insulin threshold diagram |
Here's a scary quote:
"The mixed fat and carbohydrate intake of humans allows dietary fat to supply lipid for storage in a more energy efficient process than would be achieved if significant lipogenesis from carbohydrate occurred (i.e. 2 vs. 23% of ingested calories)..."(2)
Who wants to store lipid in an "energy efficient process," at least in the modern world? Yikes! Again, junk fats and refined carbs are generally not your friends. But don't take my word for it. Sometimes it helps to actually visualize what can happen in a person's "plumbing" after a fatty meal, or even a fasted state if his glucose metabolism gets bad enough. This is not an issue reserved for textbooks and geeky theorists. It's all too real; you just usually can't see it.
But now you can. Here's a comparison of actual fasting morning blood (serum separated) drawn from a healthy athlete versus a hyper-triacylglycerol (hyper-TAG, "fatty blood"), insulin-resistant guy...
 |
The nice, clear amber-looking serum on the left is obviously preferable, yet the literally creamy, viscous serum on the right actually runs through lots of Americans' veins (and arteries). Ugh! (By the way, this is not a sample from the out-of-control diabetic I mentioned earlier.) And here's another anecdote to further illustrate: My sister, who is a surgeon, said she's operated on individuals whose blood was so thick with fat that it looked like pink foam upon making her incisions. Double Ugh! That's enough to make you ditch junk food forever, eh?
But back to the muscle versus fat thing... Body fat is certainly not meant to be the sole recipient of circulating fatty acids and glucose. Partly because of how prevalent it is in the body, it's MUSCLE that's the primary site of glucose deposition (as glycogen) in healthy situations.(2,12) (We won't worry about liver glycogen storage and production right now.)
Our dozens of kilos of muscle mass act as a "normal" glucose deposition site but don't have the same capacity to ramp up glucose uptake (in the face of screaming insulin concentrations) as our adipose tissue does. Why are we so cursed? Because our evolving ancestors, from whom you got your genetic makeup, didn't experience unnatural modern-day insulinogenic nightmares like pastries, soft drinks and Coco Puffs. Where in the natural world could you find foods that allow for a readily consumable hundred grams of sugar or more? Yet it's easy to do nowadays.
In stark contrast, our nomadic ancestors walked all day long (facilitating muscle glucose uptake [4]) and hunted/ foraged/ grazed on foods that were whole, often raw, portion-controlled (out of necessity but also good [5, 11]) and/ or were low-glycemic index.
Knowing this, why would one eat 100 g refined carbs and get his insulin up near 100 mU/L (preferable fasting insulin = 1-15 mU/L) when, during non-exercise periods, it's FAT that's going to be the greediest recipient of much of that blood sugar? Listen, insulin plays an important role in stimulating "lipoprotein lipase" (LPL, the enzyme that frees fatty acids from chylomicrons and VLDL in the circulation) AND has a direct stimulatory effect on those free fatty acids' uptake by adipocytes.(2) Can you say "lipogenesis" (fat building)?
That's not to say we want the sugar and fat remaining in our bloodstreams like the picture shown above, but neither do we want high insulin levels to hammer it all into our love handles! [Note: fish oils appear to have the ability to enhance LPL in muscles while decreasing it in fat cells, clearing our bloodstreams of fatty acids with the preferred recipient while improving glucose tolerance to boot!(1)]
Of course, timing is critical to nutrient partitioning, so massive carb intake and a subsequent insulin spike is actually advantageous post-exercise. Just limit it to a few hours after exercise and avoid massive blood sugar/ insulin responses altogether on "off" days.
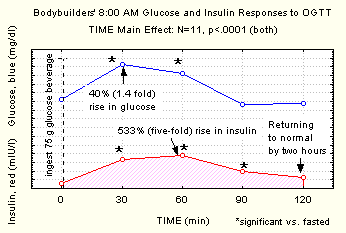 |
| Figure 2. Typical blood sugar responses to 75 g sugar in bodybuilders |
So you see, it's a management issue. When given enough insulin, pound-for-pound, fat "wins the tug-of-war" in a sense – at least at rest. Those of you who have been reading my work know that I harp on this often but here it is again: insulin is under our control like no other anabolic hormone. Use this power!
Testosterone, growth hormone, and others are just more stubbornly self-regulating by comparison. And regarding glucose tolerance supplements like chromium, vanadium, magnesium, pinitol and many other botanicals, we need to remember that regulating FOOD is paramount. Less exciting to some perhaps, but paramount! Getting away from excessive saturated fat intake and focusing on monounsaturates (olive oil) and specific polyunsaturates (fish oil), along with fiber and protein, make significant improvements over a period of just weeks!(1, 3, 7, 6, 8, 9, 10) As usual, dietary fat is a huge factor. As noted by Louheranta and colleagues: "Both the amount and quality of dietary fat can modify glucose and insulin metabolism."(6) Nice!
Well, that's enough to digest (pun intended) for now. Tune in for Part 2 next week where we discuss ways we can attempt to control insulin's indiscriminate anabolic functions and end up harnessing Mr. Hyde's powers for good.
References
1. Baltzell, J., Lipoprotein lipase in rats fed fish oil: apparent relationship to plasma insulin levels. Lipids 1991 Apr;26(4):289-94.
2. Brodsky, I. Hormone, cytokine and nutrient interaction. In: Shils, M., et al. (Eds.) Modern Nutrition in Health and Disease. Philadelphia, PA: Lippincott Williams and Wilkins. 699-704.
3. Giacco, R., et al. Dietary fibre in treatment of diabetes: myth or reality? Dig Liver Dis. 2002 Sep;34 Suppl 2:S140-4.
4. Ivy, J. The insulin-like effect of muscle contraction. Exerc Sport Sci Rev 1987;15:29-51.
5. Jenkins, D., et al. (1989). Nibbling versus gorging: metabolic advantages of increased meal frequency. N Engl J Med 321(14): 929-934.
6. Lauheranta, A., et al. Association of the fatty acid profile of serum lipids with glucose and insulin metabolism during 2 fat-modified diets in subjects with impaired glucose tolerance. Am J Clin Nutr. 2002 Aug;76(2):331-7.
7. Layman, D., et al. (2003). A reduced ratio of dietary carbohydrate to protein improves body composition and blood lipid profiles during weight loss in adult women. J Nutr 133(2): 411-417.
8. Ou, S. In vitro study of possible role of dietary fiber in lowering postprandial serum glucose. J Agric Food Chem. 2001 Feb;49(2):1026-9.
9. Parcell, A., et al. The effect of encapsulated soluble fiber on carohydrate metabolism during exercise. Int J Sport Nutr. 1999 Mar;9(1):13-23.
10. Rasmussen, O. Favourable effect of olive oil in patients with non-insulin-dependent diabetes. The effect on blood pressure, blood glucose and lipid levels of a high-fat diet rich in monounsaturated fat compared with a carbohydrate-rich diet. Ugeskr Laeger 1995 Feb 20;157(8):1028-32.
11. Speechly, D. and Buffenstein, R. (1999). Greater appetite control associated with an increased frequency of eating in lean males. Appetite 33(3): 285-297.
12. Vessby, B. Dietary fat and insulin action in humans. Br J Nutr. 2000 Mar;83 Suppl 1:S91-6.




